What can we learn from students taking part in testing?
Jim is an Associate Editor (SUs) at Wonkhe
Tags
As such even though there’s not much sign of it, proper evaluation of what has happened this term to inform national and institutional policy next term still feels important – partly because temporal proximity to vaccination is likely to lead to riskier behaviours. Are we, for example, working out who is and isn’t volunteering to get tested in this pre-Christmas period and why?
Partially stepping into the void come a couple of evaluations from late summer – one from the Norwich testing initiative and the other from Nottingham’s trial of its asymptomatic testing service – both subsequently rolled out in full.
The Norwich trial piloted mass testing on the university’s research park to assess the feasibility and acceptability of scaling up testing to all staff and students. Participants included both staff and students – although what the paper doesn’t make clear is the NRP is quite detached from UEA, and the types of students hanging out there over the late summer (mainly PG, mainly STEM researchers at that) were the sort you’d put money on to take part.
Nevertheless there was a high level of participant engagement with the study, it demonstrated that clear, consistent communications and an intuitive web application are necessary for helping participants to understand the need for testing, and indicated that universal testing on a university campus is both feasible and acceptable to the population. A roll out on the main campus ensued – so it will be interesting to see how demand held up for voluntary testing throughout the term (and who it held up with) given that looks set to be announced as the plan for next term right across the country.
Frustratingly, in this study while there was no significant demographic difference between those enrolled but did not participate and those who did participate, we don’t know if there were differences between those who did and didn’t enrol, which feels important given only 19 per cent of the eligible population enrolled.
Meanwhile in Nottingham (and the usual caveats apply here – this is a pre-print that has not yet been peer reviewed) a trial of what became its asymptomatic testing service was run over the summer at its (fairly remote) Sutton Bonington campus. A small cohort of veterinary students and staff were invited to give all of the tests a whirl – swab, saliva and finger prick – over a twelve week period, with uptake, adherence, acceptability and both students’ mental health and risk perceptions all under the spotlight.
Student characteristics weren’t a factor in predicting participation here either, but those who opted not to take part in the pilot programme reported a lower perceived risk of Covid-19 than pilot participants pre-(July) and post-pilot (October) compared with those who had taken part. It would be fascinating for obvious reasons to see if similar reasons were there in Nottingham’s roll out this last term and across the UK in this pre-Christmas “exit testing” project we have on.
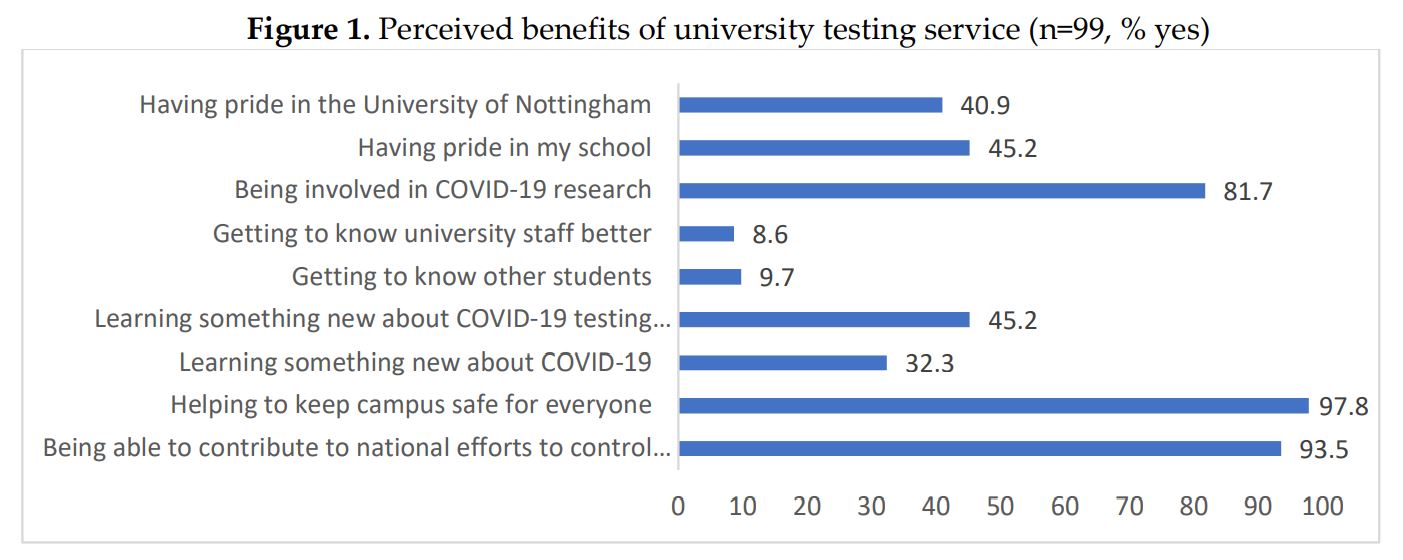
The flipside to that is the concept of “testing freedom”. Some view the idea that people will be able (either informally or formally) to go about their business free of (some) of the restrictions as a motivator for encouraging people to get a test – others would say that unless the testing is highly accurate, this is actually a problem, because it breeds complacency. What the Nottingham pilot tells us is that taking part:
Engendered a practical freedom whereby individuals felt that participation in the testing would allow them to visit family members, or made them feel more comfortable to take part in general social activities”
Later for example, one student says:
Yes I think there has been a few times when I have gone home just for the day to see my family and what not, which I probably wouldn’t have done if the testing wasn’t in place so in that regard it has like changed my behaviour in sort of that way
There are fascinating threads about mental health and wellbeing. Students and staff that took part referred to a diverse range of positive impacts on mental wellbeing – including reassurance about their personal health status, increased perception of safety on campus, reduced anxiety, increased confidence and greater feelings of satisfaction and support from the university during the pandemic.
And testing adherence was directly related to positive mental wellbeing – yet mental wellbeing was in and of itself largely associated with students’ personal concerns about themselves or their families contracting the virus.
Treading the fine line between reducing the mental wellbeing harms associated both with Covid messaging and self-isolation/distancing rules, and ensuring that students are still, on some level or another, “scared” of the virus feels like a difficult line to tread.
Finally, participants referred to a diverse range of coping mechanisms adopted in response to the virus – which included participation in the asymptomatic testing provision, media avoidance, distractions, and an acceptance that outcomes were beyond their control, all of which appeared to reduce their anxiety.
Crucially, many students referenced peer support both with relation to shared engagement with peers in the testing processes (e.g. within household “bubbles”) and accessing support from peers during self-isolation, and it was suggested that students who live off campus may have less peer support and may find periods of self-isolation more challenging than those living in halls.
Many universities have found providing support to students off-campus much more challenging than sorting services for those in halls this term, but this represents (yet) another call to redouble efforts for students in private halls and HMOs – particularly if mental wellbeing is a predictor of testing participation as well as a concern arising from restrictions.

